You could be a
for
Schedule your visit today to receive a precise diagnosis and treatment plan from our award-winning physicians!
SI Joint Stabilization
Minimally Invasive.
Non-Surgical.
The SI (Sacroiliac) Joint Stabilization procedure offers several benefits compared to traditional SI joint surgery:
- Safe posterior approach away from nerves and large blood vessels
- No metal implanted
- Fast recovery time
- Proven effective results
Common device manufactures include LinQTM and CornerLoqTM.
Frequently Asked Questions
About SI Joint Stabilization (Fusion)
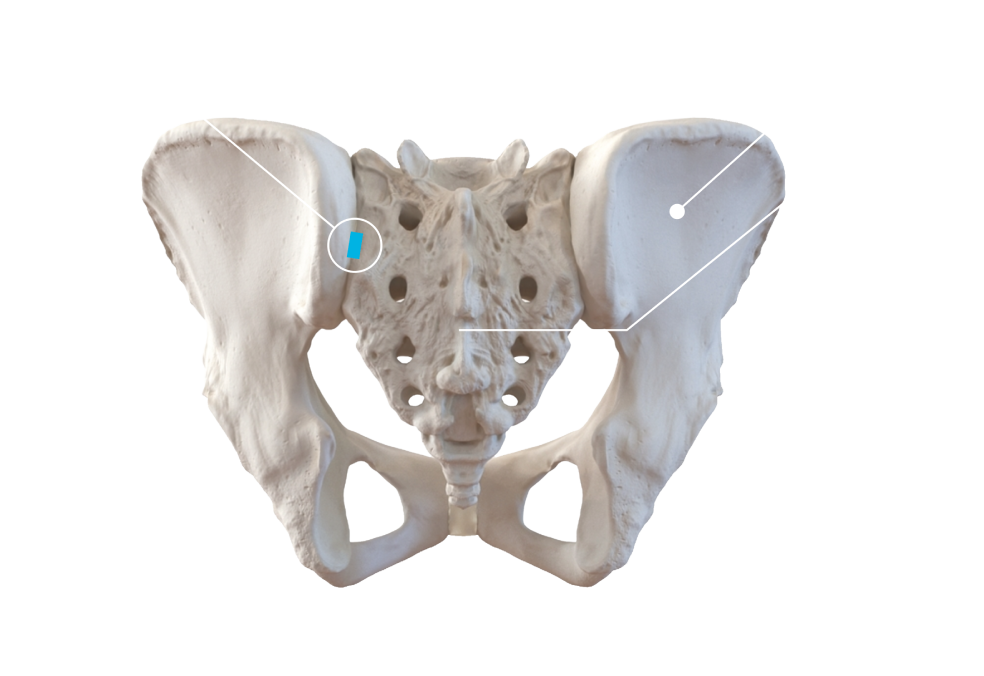
The sacroiliac joint or SI joint (SIJ) is the joint between the sacrum and the ilium bones of the pelvis, which are connected by strong ligaments. They sit on the left and right side of your spine. The primary role of the SI joint is to provide stability for the pelvis and to bear the load of the upper body when you stand or walk and shift that load to your legs. It is an essential component for energy transfer (or shock absorber) between the legs and the torso.
Common problems of the sacroiliac joint are often called sacroiliac joint dysfunction (also termed SI joint dysfunction; SIJD). Your physician may also refer to sacroiliac joint pain by other terms like sacroiliitis, SI joint degeneration, SI joint inflammation, SI joint syndrome, SI joint disruption, SI joint insufficiency, SI joint strain and arthritis.
Sacroiliac joint dysfunction generally refers to pain in the sacroiliac joint region that is caused by abnormal motion in the sacroiliac joint, either too much or too little motion due to the lack of support from the once strong and taut ligaments. In fact, research suggests the SI joint is the source of pain up to 30 percent of people with chronic low back pain. (Rashbaum, J Spinal Disord, 2016)
Low back pain is a common symptom that affects many people during their lifetime. For some, low back pain can be an acute, short-term problem. Others experience chronic, long-term symptoms that can limit mobility and effect their quality of life. Either way, the cause may or may not be your SI joint.
SI joint disorders require appropriate interpretation of your history, clinical exam results, and imaging studies. Often hip pathology and/or lumbar pathology can coexist with SI joint pathology. A healthcare provider trained in diagnosis and treatment can help diagnose your condition accurately and get you on the path for lasting relief.
To determine whether your pain is caused by your SI joint or another source, talk to a trained physician.
- Mechanical SI Joint (SIJ) dysfunction usually causes a dull unilateral low back pain (and possibly the leg and buttock).
- SIJ Pain can present as sciatica-like symptoms – such as leg pain, burning, numbness and tingling – that mimic discogenic or radicular low back pain.
- The pain is often a mild to moderate ache around the dimple or posterior superior iliac spine (PSIS) region.
- The pain may become worse and sharp while doing activities and can be triggered by standing up from a seated position or lifting the knee towards the chest during stair climbing or walking uphill.
- Pain is typically on one side or the other (unilateral PSIS pain), but the pain can occasionally be bilateral.
- You may notice that it bothers you more in the morning and gets better during the day.
- When the pain of SIJ dysfunction is severe, there can be referred pain into the hip, groin, and occasionally down the leg, but rarely does the pain radiate below the knee.
- Muscle tightness and tenderness in your hips or buttocks.
- Pain can be referred from the SIJ down into the buttock or back of the thigh, and in rare occasions, to the foot.
- Low back pain and stiffness, often unilateral, that often increases with prolonged sitting and prolonged walking.
- Disturbed sleep patterns and disturbed sitting patterns due to pain (unable to sit for long periods, sitting onone side).
- Feeling of leg instability (buckling, giving way).
The pain starts when your SI joint becomes inflamed. There are several reasons it could happen, but Hypermobility (too much movement, the joint is too loose) and Hypomobility (too little movement) are at the root of the problem.
Hypermobility: The ligaments that encase the SI joint may be disrupted due to injury or degenerate due to age, allowing the joint to have excessive motion. This excessive motion may inflame and disrupt the joint and surrounding nerves.
Hypomobility: Often caused by arthritis, this triggers the bones to rub against one another and create extreme pain and may inhibit mobility.
- A traumatic event or impact: either a combination of vertical compression and rapid rotation (i.e. carrying a heavy object and twisting), or an impact, such as car accident or a fall. Pain can occur suddenly or can develop over time (degeneration).
- Pregnancy: Hormones are released to loosen ligaments and joints to prepare for childbirth, which changes the way the SI joint moves and makes it less stable. Extra weight also puts more stress on the SI joints, leading to additional wear.
- Abnormal walking pattern: If one leg is shorter than the other, or you favor one leg when you walk because of pain, it can lead to SI joint pain.
- Spine surgeries: Fusing vertebrae reduces flexibility in the spine, which can increase stress on the SI joint.
- Infection: In rare cases, the SI joint can become infected and degenerate.
- Previous iliac crest bone graft. (ICBG)
- Wear-and-tear arthritis (osteoarthritis) can occur in sacroiliac joints, as can ankylosing spondylitis — a type of inflammatory arthritis that affects the spine.
SI Joint Fusion is covered by most health insurance plans including Medicare, Medicaid (varies by state), most workers’ compensation plans, and most commercial payers. Our team will verify your eligibility for coverage prior to your procedure.
Start Living Pain Free!
The day of your procedure
Sacroiliac (SI) joint fusion is a surgical procedure performed in an operating room, with either general anesthesia or MAC (monitored anesthesia care). The LinQ Implant System, a minimally invasive surgical (MIS) procedure, requires a small incision (about one to two inches long), in the lower back.
The LinQ procedure involves the insertion of a small bone allograft implant in the SI joint and is designed to stabilize and fuse the SI joint. This procedure is done through a single, small incision in your lower back and is usually completed in less than one hour.

Post-operative expectations
The whole LinQ SI procedure usually takes less than an hour, and recovery time is significantly less than most conventional SI Fusion Surgeries.
In a typical situation, patients walk out of the hospital or surgery center soon after they have recovered from anesthesia.
There are some light restrictions and your surgeon will arrange a follow-up visit to assess your progress and health status (including the status of your incision) and may take additional x-rays of your surgical site if necessary. When you return to work and resume other activities will depend on your postsurgical progress and occupation.
Real Patient Stories






HAVE A QUESTION?
You deserve guidance and support, we're here to help
- Free 20-minute call with a Care Coordinator
- Ask questions and discuss candidacy
- The fastest way to schedule with a specialist
We'd love to chat
Our team is happy to help with any questions you may have. We are available for calls and live chat during typical business hours, and you can always communicate with us at your convenience.


